Autonomic Innervation of the Heart and Vasculature
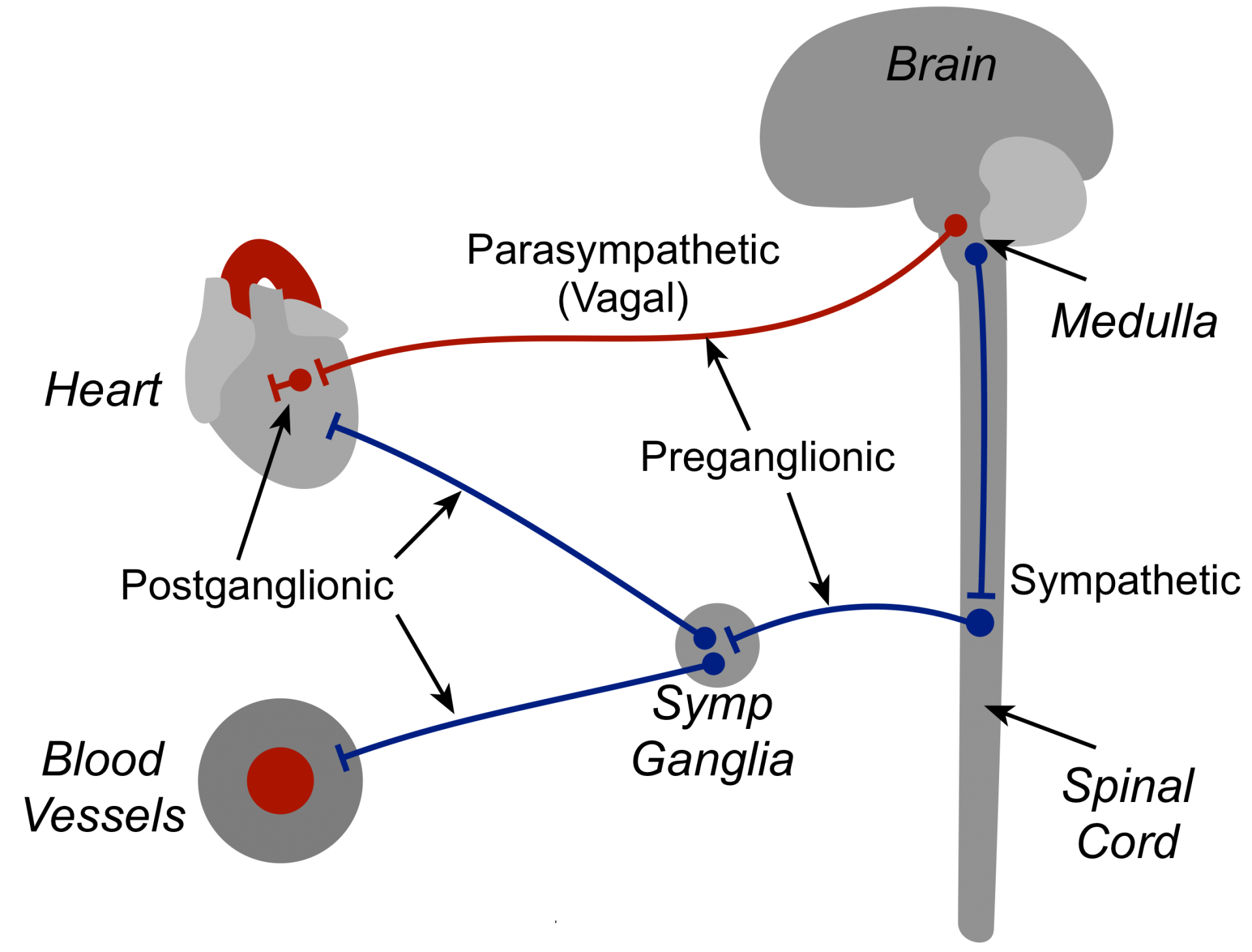
The medulla, located in the brainstem above the spinal cord, is a major site in the brain for regulating autonomic nerve outflow to the heart and blood vessels, and is important for short-term feedback regulation of arterial pressure. The medulla contains cell bodies for the two main divisions of the autonomic nervous system - sympathetic and parasympathetic. The sympathetic nerves exit the medulla and travel down the spinal cord where they synapse with relatively short preganglionic fibers that travel to, and synapse within, sympathetic ganglia. Postganglionic efferent fibers from the ganglia travel to the heart and vasculature, where they synapse at their target sites. The parasympathetic nerves (vagus nerves, cranial nerve X) exit the medulla as long preganglionic efferent fibers that form synapses with short postganglionic fibers within the heart or vascular tissue. The activity of the medullary neurons is modulated by input from peripheral sensors and from other brain regions.
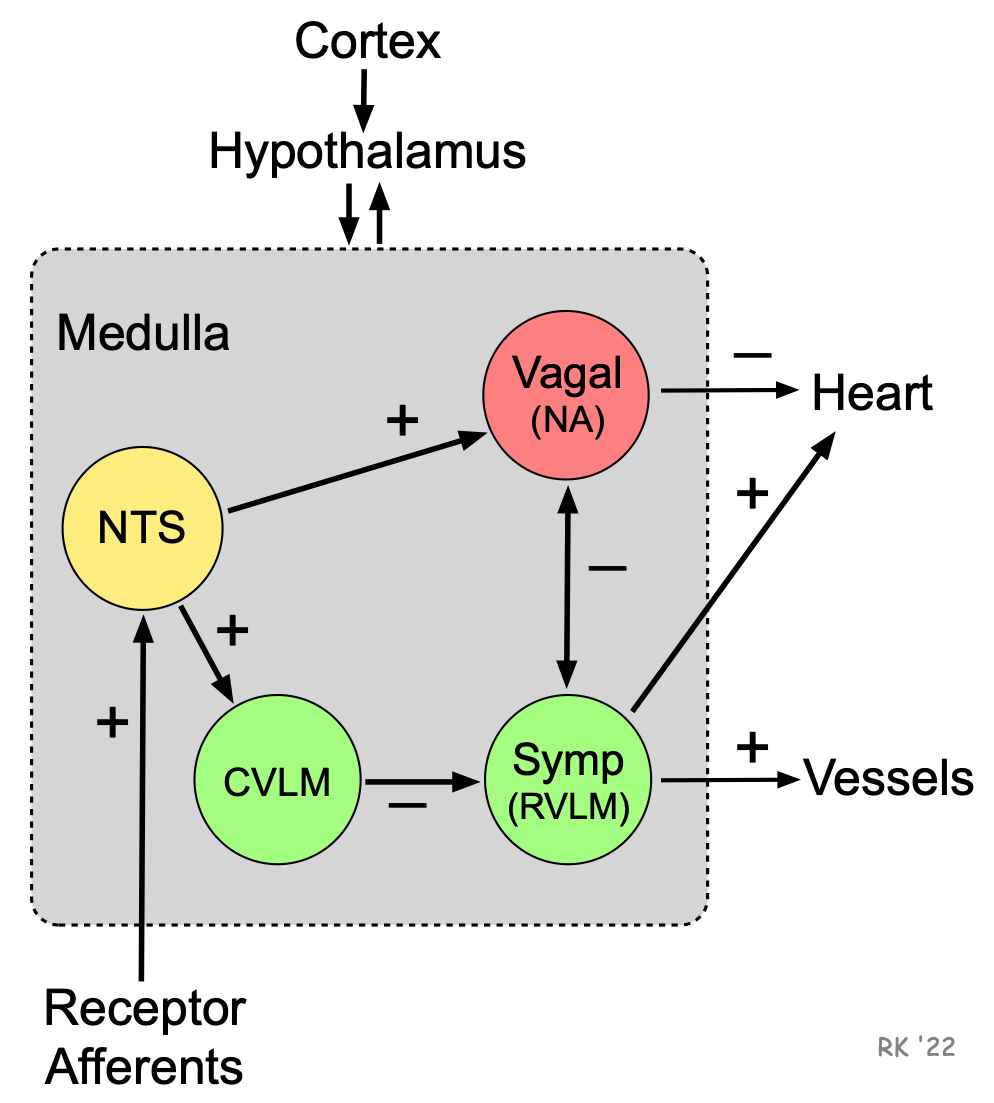 The nucleus tractus solitarius (NTS) of the medulla receives sensory input from different systemic and central receptors (e.g., baroreceptors and chemoreceptors). Neural connections from the NTS modulate the activity of sympathetic neurons in the rostral ventrolateral medulla (RVLM) (via the caudal ventrolateral medulla, CVLM), and the activity of parasympathetic neurons in the nucleus ambiguus (NA) from which arise the parasympathetic vagus nerves (tenth cranial nerves). Neuronal activity in the NTS activates (+) vagal neurons and inhibits (-) sympathetic neurons. The medulla also receives information from other brain regions (e.g., hypothalamus). The hypothalamus and higher centers modify the activity of the medullary centers and are important in stimulating cardiovascular responses to emotion and stress (e.g., exercise, thermal stress). In summary, the medulla receives input from peripheral receptors and the brain, and regulates autonomic outflow from specific medullary regions via sympathetic and parasympathetic (vagal) efferent nerves, which travel to the heart and blood vessels.
The nucleus tractus solitarius (NTS) of the medulla receives sensory input from different systemic and central receptors (e.g., baroreceptors and chemoreceptors). Neural connections from the NTS modulate the activity of sympathetic neurons in the rostral ventrolateral medulla (RVLM) (via the caudal ventrolateral medulla, CVLM), and the activity of parasympathetic neurons in the nucleus ambiguus (NA) from which arise the parasympathetic vagus nerves (tenth cranial nerves). Neuronal activity in the NTS activates (+) vagal neurons and inhibits (-) sympathetic neurons. The medulla also receives information from other brain regions (e.g., hypothalamus). The hypothalamus and higher centers modify the activity of the medullary centers and are important in stimulating cardiovascular responses to emotion and stress (e.g., exercise, thermal stress). In summary, the medulla receives input from peripheral receptors and the brain, and regulates autonomic outflow from specific medullary regions via sympathetic and parasympathetic (vagal) efferent nerves, which travel to the heart and blood vessels.
The heart is innervated by vagal and sympathetic fibers. The right vagus nerve primarily innervates the SA node, whereas the left vagus innervates the AV node; however, there can be a significant overlap in the anatomical distribution. Atrial muscle is also innervated by vagal efferent nerves, whereas the ventricular myocardium is only sparsely innervated by vagal efferent nerves. Sympathetic efferent nerves are present throughout the atria (especially in the SA node) and ventricles, including the conduction system of the heart.
Sympathetic stimulation of the heart increases heart rate (positive chronotropy), inotropy, and conduction velocity (positive dromotropy), whereas parasympathetic stimulation of the heart has opposite effects. Sympathetic and parasympathetic effects on heart function are mediated by beta-adrenoceptors and muscarinic receptors, respectively.
Sympathetic adrenergic nerves travel along arteries and nerves and are found in the adventitia (outer wall of a blood vessel). Varicosities, which are small enlargements along the nerve fibers, are the site of neurotransmitter (norepinephrine) release. Capillaries receive no innervation. Activation of vascular sympathetic nerves causes contraction of the vascular smooth muscle and vasoconstriction of arteries and veins mediated by alpha-adrenoceptors.
Parasympathetic fibers are found associated with blood vessels in certain organs, such as salivary glands, gastrointestinal glands, and in genital erectile tissue. Parasympathetic nerves release of acetylcholine (ACh) that binds to muscarinic ACh receptors. This causes vasodilation through the formation of nitric oxide and subsequent guanylyl cyclase activation. ACh release can stimulate the release of kallikrein from glandular tissue that acts upon kininogen to form kinins (e.g., bradykinin). Kinins cause increased capillary permeability and venous constriction, along with arterial vasodilation in specific organs.
See Cardiovascular Actions of Autonomic Nerve Activation
Revised 09/09/22

 Cardiovascular Physiology Concepts, 3rd edition textbook, Published by Wolters Kluwer (2021)
Cardiovascular Physiology Concepts, 3rd edition textbook, Published by Wolters Kluwer (2021) Normal and Abnormal Blood Pressure, published by Richard E. Klabunde (2013)
Normal and Abnormal Blood Pressure, published by Richard E. Klabunde (2013)