Vascular Tone
 Vascular tone refers to the degree of constriction experienced by a blood vessel relative to its maximally dilated state. All arterial and venous vessels under basal conditions exhibit some degree of smooth muscle contraction that determines the diameter, and hence tone, of the vessel.
Vascular tone refers to the degree of constriction experienced by a blood vessel relative to its maximally dilated state. All arterial and venous vessels under basal conditions exhibit some degree of smooth muscle contraction that determines the diameter, and hence tone, of the vessel.
Basal vascular tone differs among organs. Those organs having a large vasodilatory capacity (e.g., myocardium, skeletal muscle, skin, splanchnic circulation) have high vascular tone, whereas organs having relatively low vasodilatory capacity (e.g., cerebral and renal circulations) have low vascular tone.
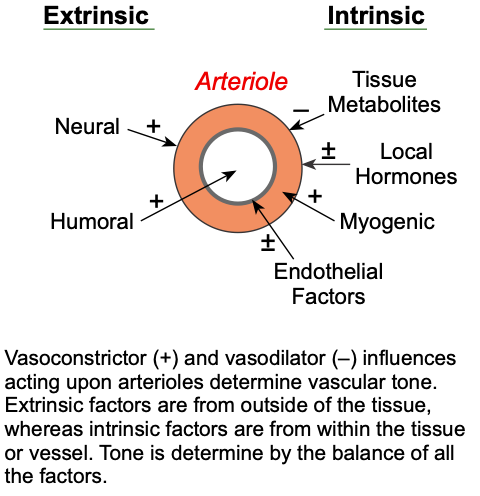
Vascular tone is determined by many competing vasoconstrictor and vasodilator influences acting on the blood vessel. These influences can be separated into extrinsic factors that originate from outside the organ or tissue in which the blood vessel is located, and intrinsic factors that originate from the vessel itself or the surrounding tissue. The primary function of extrinsic factors is to regulate arterial blood pressure by altering systemic vascular resistance, whereas intrinsic mechanisms are important for local blood flow regulation within an organ. Vascular tone is determined by the balance of competing vasoconstrictor and vasodilator influences.
Extrinsic factors (neurohumoral) such as sympathetic nerves and circulating angiotensin II increase vascular tone (i.e., cause vasoconstriction); however, some circulating factors (e.g., atrial natriuretic peptide) decrease vascular tone. Intrinsic factors include:
- Myogenic mechanisms (originating from vascular smooth muscle), which increase tone.
- Endothelial factors, such as nitric oxide and endothelin, can either decrease or increase tone, respectively.
- Local hormones/chemical substances (e.g., arachidonic acid metabolites, histamine, and bradykinin can either increase or decrease tone.
- Metabolic by-products or hypoxia, which decrease tone.
The mechanisms by which the above influences either constrict or relax blood vessels involve various signal transduction mechanisms that ultimately influence the interaction between actin and myosin in the smooth muscle.
Revised 11/03/2023

 Cardiovascular Physiology Concepts, 3rd edition textbook, Published by Wolters Kluwer (2021)
Cardiovascular Physiology Concepts, 3rd edition textbook, Published by Wolters Kluwer (2021) Normal and Abnormal Blood Pressure, published by Richard E. Klabunde (2013)
Normal and Abnormal Blood Pressure, published by Richard E. Klabunde (2013)