Factors Promoting Venous Return
Skeletal Muscle Pump
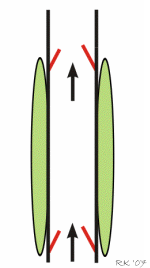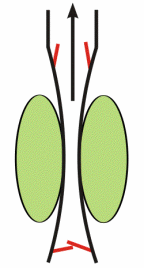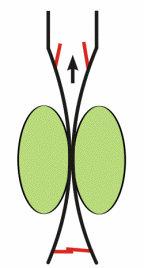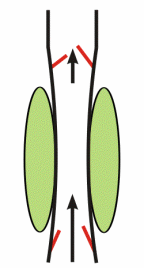 A major mechanism promoting venous return during normal locomotory activity (e.g., walking, running) is the muscle pump system. Peripheral veins, particularly in the legs and arms, have one-way valves that direct flow away from the limb and toward the heart. Veins physically located within large muscle groups undergo compression as the muscles surrounding them contract, and they become decompressed as the muscles relax. Therefore, with normal cycles of contraction and relaxation, the veins are alternately compressed and decompressed (i.e., "pumped"). As illustrated in the animated figure, muscle contraction propels blood forward through the open distal valves (upper valves in figure) and impedes flow into the muscle as the proximal valves close during contraction (lower valves in figure). During muscle relaxation, the proximal valves open and blood flows into and fills the venous segment. Initially, during relaxation, the distal valves close, but then they open as the volume of blood and pressure increases in the venous segment. The net effect is that the cycle of compression and relaxation propels the blood in the heart's direction. Venous valves prevent the blood from flowing backwards, permitting unidirectional flow that enhances venous return. When a person is standing, postural muscles in the legs alternately contract and relax to keep the body in balance. This muscle activity promotes venous return and helps to maintain central venous pressure and venous return, and lowers venous and capillary pressures in the feet and lower limbs.
A major mechanism promoting venous return during normal locomotory activity (e.g., walking, running) is the muscle pump system. Peripheral veins, particularly in the legs and arms, have one-way valves that direct flow away from the limb and toward the heart. Veins physically located within large muscle groups undergo compression as the muscles surrounding them contract, and they become decompressed as the muscles relax. Therefore, with normal cycles of contraction and relaxation, the veins are alternately compressed and decompressed (i.e., "pumped"). As illustrated in the animated figure, muscle contraction propels blood forward through the open distal valves (upper valves in figure) and impedes flow into the muscle as the proximal valves close during contraction (lower valves in figure). During muscle relaxation, the proximal valves open and blood flows into and fills the venous segment. Initially, during relaxation, the distal valves close, but then they open as the volume of blood and pressure increases in the venous segment. The net effect is that the cycle of compression and relaxation propels the blood in the heart's direction. Venous valves prevent the blood from flowing backwards, permitting unidirectional flow that enhances venous return. When a person is standing, postural muscles in the legs alternately contract and relax to keep the body in balance. This muscle activity promotes venous return and helps to maintain central venous pressure and venous return, and lowers venous and capillary pressures in the feet and lower limbs.
Respiratory Activity (Abdominothoracic or Respiratory Pump)
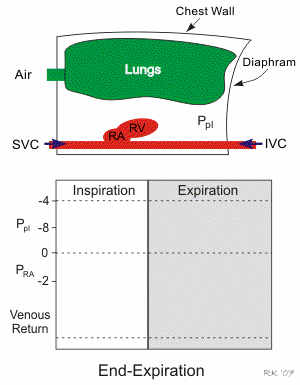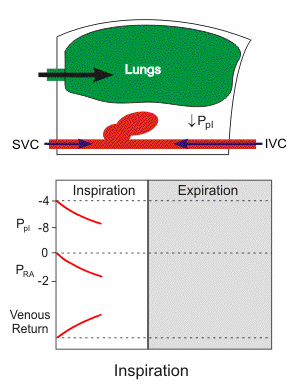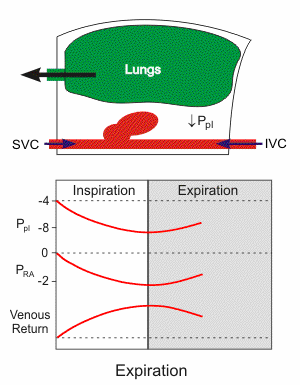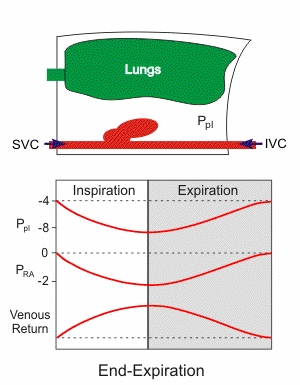 Respiratory activity influences venous return to the heart. Briefly, increasing the rate and depth of respiration promotes venous return and therefore enhances cardiac output. Non-typical respiratory activity such as being on positive pressure ventilation or doing a forced expiration against a closed glottis (Valsalva maneuver) impedes and therefore reduces venous return and cardiac output.
Respiratory activity influences venous return to the heart. Briefly, increasing the rate and depth of respiration promotes venous return and therefore enhances cardiac output. Non-typical respiratory activity such as being on positive pressure ventilation or doing a forced expiration against a closed glottis (Valsalva maneuver) impedes and therefore reduces venous return and cardiac output.
Respiratory activity affects venous return through changes in right atrial pressure, which is an important component of the pressure gradient for venous return. Increasing right atrial pressure impedes venous return, while lowering this pressure facilitates venous return. Respiratory activity can also affect the diameter of the thoracic vena cava and cardiac chambers, which either directly (e.g., vena cava compression) or indirectly (by changing cardiac preload) affect venous return.
Pressures and volumes in the right atrium and thoracic vena cava depend on intrapleural pressure (Ppl), which is the pressure within the thoracic space between the organs (lungs, heart, vena cava) and the chest wall. During inspiration, the chest wall expands, and the diaphragm descends (see the animated figure). This makes the Ppl become more negative, which leads to expansion of the lungs, cardiac chambers (right atrium [RA] and right ventricle [RV]), and the thoracic superior and inferior vena cava (SVC and IVC, respectively). This expansion causes the intravascular and intracardiac pressures (e.g., right atrial pressure) to fall. Because the pressure inside the cardiac chambers falls less than the Ppl, the transmural pressure (pressure inside the heart chamber minus the Ppl) increases, which leads to cardiac chamber expansion and an increase in cardiac preload and stroke volume through the Frank-Starling mechanism. As right atrial pressure falls during inspiration, the pressure gradient for venous return to the right ventricle increases. During expiration, the opposite occurs, although the dynamics are such that the net effect of respiration is that increasing the rate and depth of ventilation facilitates venous return and ventricular stroke volume.
The left side of the heart responds differently to the respiratory cycle. During inspiration, expansion of the lungs and pulmonary vessels causes pulmonary blood volume to increase, which transiently decreases the flow of blood from the lungs to the left atrium. Therefore, left ventricular filling actually decreases during inspiration. In contrast, during expiration, lung deflation causes flow to increase from the lungs to the left atrium, which increases left ventricular filling. The net effect of increased rate and depth of respiration, however, is an increase in left ventricular stroke volume and cardiac output.
Revised 01/23/2023

 Cardiovascular Physiology Concepts, 3rd edition textbook, Published by Wolters Kluwer (2021)
Cardiovascular Physiology Concepts, 3rd edition textbook, Published by Wolters Kluwer (2021) Normal and Abnormal Blood Pressure, published by Richard E. Klabunde (2013)
Normal and Abnormal Blood Pressure, published by Richard E. Klabunde (2013)